There are many skin disorders, with or without itchiness, which can affect humans, to a greater or lesser extent. For information, diagnosis or treatment for your skin problems, Eucare invites its patients to seek a doctor’s opinion. In this article we present some of the main skin disorders.
Psoriasis: one of the most frequent skin diseases
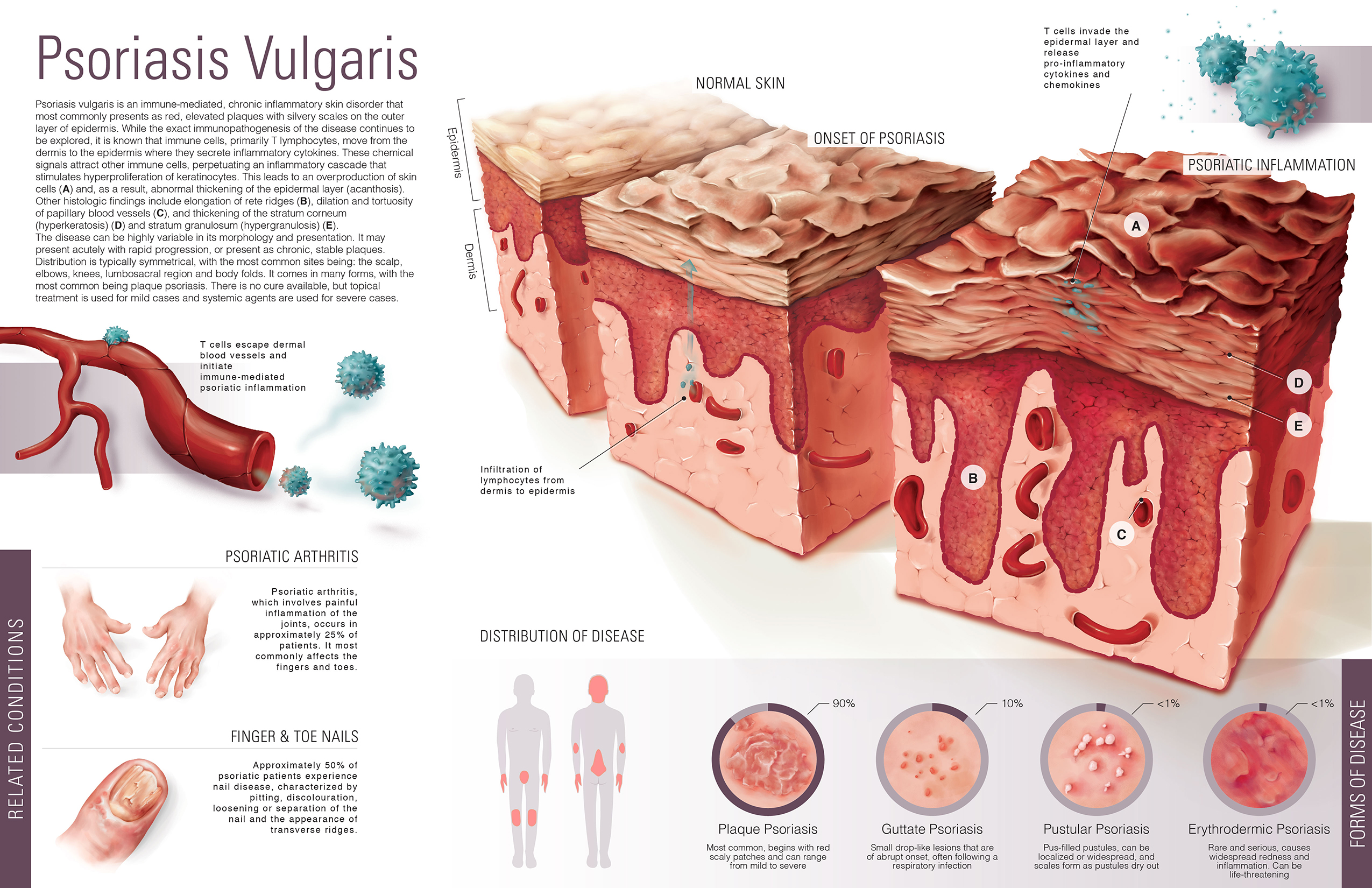
Most people have heard about psoriasis, being one of the most well-known skin disorders and considering that it is quite common and difficult to treat. It is a chronic and recurrent inflammation but is neither infective nor contagious. It is triggered in the immune system: T lymphocytes (white blood cells with the function of identifying and attacking foreign bodies or substances) stimulate the skin to produce excess cytokines creating abrasions. In around a third of cases it is a hereditary disease. It is said to be a chronic inflammation, but it can improve and then reoccur. Relapse can depend on each individual's condition. Relapse is triggered by stress, infections, climate changes, medicines and in particular the use of antidepressants containing lithium.
Psoriasis presents itself in different forms, the most common typically presents with red patches with white scales on top.
These patches can present themselves on different parts of the body and can be widely or less widely spread. In some cases the typical eruptions of psoriasis can also be pustular, that is,contain pus. Other forms are inverse psoriasis- in this case the skin eruptions can be found in areas which are frequently rubbed those surrounding the genitals, under arms and under breasts. Guttate psoriasis is caused by streptococcus and erythrodermic psoriasis, from burns or medicines and usually gives itchiness.
There are different treatments possible which a dermatologist will evaluate based on the type and seriousness of the psoriasis. The mildest treatment is topical treatment with cortisone and there are also treatmentswith vitamin D3 available, which regulate the excessive production of cells. In both cases the disorder may regress and the psoriasis improve, but it rarely completely disappears. Another solution is exposure to UV rays, both type A and type B. The effects can be strengthened with the use of photosensitising medications which make the body more sensitive to the exposure of UV rays. In this case it is important to be aware of the contraindications as it may increase the risk of tumours. A third possibility is systemic treatment using different types of immunosuppressive medication.
Seborrheic Dermatitis: Skin disorders
You have most probably also heard about seborrheic dermatitis as it is a rather common condition which mainly affects the scalp, however the armpits, inguinal area, ears and eyebrows are also often affected. How can you recognise it? It presents as an inflammation with reddening and itchiness. Seborrheic dermatitis is caused by a fungus called Malassezia furfur which causes irritation to the skin. Following the flaking which is caused by irritatation the cells produce scales which are often greasy and yellowish.
As with psoriasis, seborrheic dermatitis also has a high incidence due to heriditary factors, however it can also occur in case of stress, hormonal variations, use of corticosteroids, excessive heat, humidity, poor hygiene, trichotillomania (the habit of constantly touching hair). Unlike psoriasis, seborrheic dermatitis can be easily overcome using specific products, such as fungicideshampoos.
White patches on the skin? It could be vitiligo
Here is another skin disease which you have probably heard about: vitiligo. It is a continual long-term and progressive disease, meaning that once it has appeared, the condition of the skin tends to worsen and thus
it is necessary to find a solution to slow down the progression of the disease or to camouflage and reduce the antiaesthetic effects. Vitiligo is characterised by the presence of patches on the skin which are very light in colour, from white to pale pink. It occurs when some skin cells stop producing melanin. Vitiligo affects people independently of their sex, race and age, however it is more evident in people with dark skin. Concerning its possible causes, it is often associated with autoimmune disorders such as thyroiditis, atrophic gastritis, diabetes.
It can be classed into different types:
– Focal Vitiligo with only a few macules in a small area of the skin;
– Segmental vitiligo which affects only one side of the body, for example a leg or an arm (rare);
– Generalized Vitiligo distributed in a rather uniformly way on different parts of the body;
– Universal Vitiligo when the whole body is affected.
With regard to treatment, it is possible to use sun creams which avoid some areas becoming darker than others, topical medication with cortisone which can favour, in the initial phase, a repigmentation of the lighter areas, and also photo-chemotherapy with type A ultraviolet rays which stimulates the production of melanin. In this case, before exposure to UV rays it is necessary to administer a photosensitising drug.
Scabies: a contagious skin disease
Among the most wide spread skin diseases which you will have heard about, there is scabies. It is an infection of the skin characterised by painful blisters caused by microscopic mites which burrow into the skin where they deposit eggs. Scabies is visible to the naked eye as reddish lines on the skin, particularly in areas around the wrists and fingers, but also in feet and armpit areas. The symptoms of scabies are itchiness, which causes the affected person to scratch which consequently results in crusts and scaly skin.
Unlike the skin diseases seen so far, scabies is contagious and therefore one has to be careful for example when sharing towels, skin contact and in sexual relationships (in this case the use of a condom is not sufficient). Although it is more irritating compared to other skin disorders, scabies, unlike those looked at so far, can be cured definitively through the use of specific creams. The latter are to be administered only following a positive diagnosis by a dermatologist, after having taken a sample of the skin to be examined under a microscope.
Eucare does not enter into doctor-patient relationship. All information published by PharmaRoma does not express a medical opinion. For visits, diagnosis or accurate prevention, contact a specialist doctor.











 Free Shipping for Orders Above € 120
Free Shipping for Orders Above € 120